Nature versus nurture. When it comes to health, both exert powerful influence. To what extent does a particular disease—diabetes in children, say, or cancer in the elderly—arise from genetic baggage beyond our control, and to what degree does it result from modifiable environmental and “lifestyle†choices? While most disorders result from a combination of both genetic and environmental factors, researchers say parsing out the roles of these two players is complicated business.
Nature versus nurture. When it comes to health, both exert powerful influence. To what extent does a particular disease—diabetes in children, say, or cancer in the elderly—arise from genetic baggage beyond our control, and to what degree does it result from modifiable environmental and “lifestyle” choices? While most disorders result from a combination of both genetic and environmental factors, researchers say parsing out the roles of these two players is complicated business.
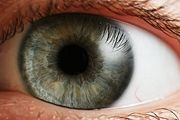
But according to one new study of the common eye disease known as age-related macular degeneration (AMD), it’s possible to characterize and quantify the interplay between genes and lifestyle. By taking advantage of both Human Genome Project data and ongoing cohort studies, David Hunter, director of the Harvard School of Public Health’s Center for Cancer Prevention, and Debra Schaumberg, an associate professor at Harvard Medical School and director of Ophthalmic Epidemiology at Brigham and Women’s Hospital, in Boston, have calculated the incremental increases in people’s AMD risk, depending on whether they’re affected by one mutant gene; two mutant genes; and perhaps also obesity or smoking, two common lifestyle variables.
Their findings, published in the Archives of Ophthalmology in January, illuminate the origins of AMD. Up to 15 million Americans suffer from the disorder, a leading cause of vision loss in those over age 60, according to the National Institutes of Health. As the population ages, the incidence of AMD will no doubt increase.
“We’re accounting for both sides of the ”˜nature versus nurture’ dichotomy,” says Hunter, the Vincent L. Gregory Professor in Cancer Prevention in the departments of Epidemiology and Nutrition at HSPH. “But even more important, understanding how the environment might affect a person’s genetic predisposition to a disease should help us understand the disease and its mechanisms better.”
The risks add up
!ADVERTISEMENT!
In 2005, after mining data from the Human Genome Project, researchers traced the genetic roots of AMD to inherited mutations in two genes known as complement factor H (CFH) and LOC387715. They found that, for people who carry either of these mutations, and who either smoke or are obese, AMD risk rises significantly. For example, people with the CFH mutation have a four-times higher risk than those without it. But if those same people smoke, their risk doubles, to 8.69. If they are obese, their risk rises 12-fold.
By the same token, a mutation in the LOC387715 gene increases a person’s risk for AMD 6.33 times. But if that person smokes, that risk multiplier jumps to 22.5. Surprisingly, other lifestyle factors associated with AMD, such as regular aspirin use or consumption of fruit, fatty acids, or alcohol, had no effect. (People with mutations in both LOC387715 and CFH are a staggering 50 times more likely to develop AMD, regardless of lifestyle, but such combined mutations are extremely rare.) See graphic
To calculate these odds, the investigators took advantage of two large, ongoing epidemiological studies: the Nurses’ Health Study, which began in 1976 at Brigham and Women’s Hospital, and the Health Professionals Follow-up Study, which was launched 10 years later and is based at HSPH. In both studies, participants provide DNA samples upon entering and fill out health-status questionnaires every two years. Hunter and Schaumberg collected lifestyle and health information for 882 people who had developed AMD and compared it to data from 2,056 individuals who were generally similar but did not have AMD. Thanks to the size and quality of this unique data trove, researchers are able to estimate the relative influences of genetic and lifestyle factors with a high degree of accuracy.
According to Schaumberg, “This is one of the first and finest examples of how we’ve identified the important genetic predisposing factors for a chronic age-related disease, then begun to piece together the puzzle on how genes interact with lifestyle. This study has become the paradigm for people to start talking about the genetic epidemiology of chronic disease.”
A commentary in the Journal of the American Medical Association published in January, 2007, supports Schaumberg’s claim. According to Jonathan Haines, of Vanderbilt University Medical Center, and Margaret Pericak-Vance, at the University of Miami, Hunter and Schaumberg’s paper should serve as a model for future studies of a host of disorders, from cardiovascular disease to inflammatory bowel disease. “As medical science moves further into the genomics era and closer to the widespread use of genomic medicine in individualized health care, successes such as those for AMD will become commonplace,” the authors write.
Weighing the relative impact of how genes and environment, nature and nurture, help cause diseases is only part of the goal, Hunter points out. Ultimately, he says, “we want to discover lifestyle factors that reduce disease risk.”
David Cameron, who writes about health and science, has a special interest in the genetic roots of disease.