WASHINGTON (Reuters) - Hospitals seeking to keep patients from picking up infections should focus as much on cleaning up invisible germs as on removing the visible dirt, a British doctor argued on Tuesday.
Clean hands can only go so far in protecting patients from infection if doorknobs, bed rails and even sheets are covered with bacteria and viruses, Dr. Stephanie Dancer of South General Hospital in Glasgow writes in the journal Lancet Infectious Diseases.
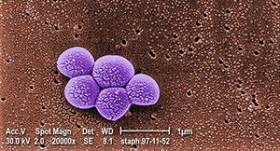
But other infection experts differed on whether clean equipment and telephones affect a patient's biggest risk of acquiring a "superbug" such as methicillin resistant Staphylococcus aureus, or MRSA.
WASHINGTON (Reuters) - Hospitals seeking to keep patients from picking up infections should focus as much on cleaning up invisible germs as on removing the visible dirt, a British doctor is arguing.
Clean hands can only go so far in protecting patients from infection if doorknobs, bed rails and even sheets are covered with bacteria and viruses, Dr. Stephanie Dancer of South General Hospital in Glasgow writes in the journal Lancet Infectious Diseases.
But other infection experts differed on whether clean equipment and telephones affect a patient's biggest risk of acquiring a "superbug" such as methicillin resistant Staphylococcus aureus, or MRSA.
The U.S. Centers for Disease Control and Prevention estimates that people get an infection while in a hospital, nursing home or other health-care facility 1.7 million times each year and that 99,000 people die from them.
Earlier this month, a report in the Journal of the American Medical Association showed that MRSA killed an estimated 19,000 Americans in 2005 and that 85 percent of them were infected in hospitals.
!ADVERTISEMENT!Experts in infectious disease are constantly urging doctors, nurses and other hospital staff to wash their hands frequently and yet infections continue to spread. "... even if everyone does wash their hands properly, the effects of exemplary hand hygiene are eroded if the environment is heavily contaminated by MRSA," Dancer wrote.
NOSE PICKING
"Given the propensity for people to pick, touch, or blow their noses, it is not surprising that carriers will often harbor their own strain of S. aureus on their fingers, which they will then transfer to any site accessible to their hands," she said.
Bacteria such as S. aureus and viruses such as the noroviruses that cause diarrhea can live on plastic or metal surfaces for days, Dancer said.
"The evidence for S. aureus and MRSA contamination of a huge variety of items in hospitals is overwhelming. Objects such as computer keyboards, door handles, tourniquets, pens, television sets, stethoscopes, telephones, beds and bedside tables, equipment packaging, paper and patient's notes, and toys are just a few examples," she wrote.
Dr. William Schaffner, of the Vanderbilt University School of Medicine and vice president of the National Foundation for Infectious Diseases, disagreed. "These inanimate surfaces are not likely to be a mode of transmission," he said in a telephone interview.
"It's close patient contact by the hands of health-care workers that go from one patient, get contaminated and go to another," he said. "Even in grubby hospital rooms -- it looks gross but it's not where the staph come from."
But Dancer's argument rang true to Dr. Ed Septimus of Methodist Hospital system in Houston, who is on the board of directors of the Infectious Diseases Society of America.
He said hospitals do not routinely clean surfaces in patient rooms except between patients, even though those surfaces could easily harbor bacteria.
"If it's on my clothes, then I could touch my clothes and then touch the patient," Septimus said in a telephone interview.
He suggested training cleaning staff better so that they do more than empty trash and clean the toilet.