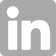Inflammation is a protective attempt by the organism to remove the injurious stimuli and to initiate the healing process Scientists have identified a protein that acts as a "master switch" in certain white blood cells, determining whether they promote or inhibit inflammation. The study, published in the journal Nature Immunology, could help researchers look for new treatments for diseases such as rheumatoid arthritis that involve excessive inflammation. Inflammatory responses are an important defense that the body uses against harmful stimuli such as infections or tissue damage, but in many conditions, excessive inflammation can itself harm the body. In rheumatoid arthritis, the joints become swollen and painful, but the reasons why this happens are not well understood.
Inflammation is a protective attempt by the organism to remove the injurious stimuli and to initiate the healing process Scientists have identified a protein that acts as a "master switch" in certain white blood cells, determining whether they promote or inhibit inflammation. The study, published in the journal Nature Immunology, could help researchers look for new treatments for diseases such as rheumatoid arthritis that involve excessive inflammation. Inflammatory responses are an important defense that the body uses against harmful stimuli such as infections or tissue damage, but in many conditions, excessive inflammation can itself harm the body. In rheumatoid arthritis, the joints become swollen and painful, but the reasons why this happens are not well understood.
!ADVERTISEMENT!
Without inflammation, wounds and infections would never heal. Similarly, progressive destruction of the tissue would compromise the survival of the organism. However, chronic inflammation can also lead to a host of diseases, such as hay fever, atherosclerosis, and rheumatoid arthritis. It is for that reason that inflammation is normally closely regulated by the body.
Inflammation can be classified as either acute or chronic. Acute inflammation is the initial response of the body to harmful stimuli and is achieved by the increased movement of plasma and leukocytes from the blood into the injured tissues.
Prolonged inflammation, known as chronic inflammation, leads to a progressive shift in the type of cells present at the site of inflammation and is characterized by simultaneous destruction and healing of the tissue from the inflammatory process.
Cells of the immune system called macrophages can either stimulate inflammation or suppress it by releasing chemical signals that alter the behavior of other cells. The new study, by scientists from Imperial College London, has shown that a protein called IRF5 acts as a molecular switch that controls whether macrophages promote or inhibit inflammation.
The results suggest that blocking the production of IRF5 in macrophages might be an effective way of treating a wide range of autoimmune diseases, such as rheumatoid arthritis, inflammatory bowel disease, lupus, and multiple sclerosis. In addition, boosting IRF5 levels might help to treat people whose immune systems are compromised.
Dr Irina Udalova from the Kennedy Institute of Rheumatology at Imperial College London, the senior researcher on the study, said:
"Diseases can affect which genes are switched on and off in particular types of cells. Understanding how this switching is regulated is crucial for designing targeted strategies to suppress unwanted cell responses.
"Our results show that IRF5 is the master switch in a key set of immune cells, which determines the profile of genes that get turned on in those cells. This is really exciting because it means that if we can design molecules that interfere with IRF5 function, it could give us new anti-inflammatory treatments for a wide variety of conditions."
They used engineered viruses to introduce extra copies of the IRF5 gene in human macrophages grown in the laboratory, making the cells produce more IRF5. When they did this to macrophages with anti-inflammatory characteristics, it made them switch to promoting inflammation. When they blocked IRF5 in pro-inflammatory macrophages using synthetic molecules, this reduced the cells' production of signals that promote inflammation.
IRF5 seems to work by switching on genes that stimulate inflammatory responses and dampening genes that inhibit them. It can either do this by interacting with DNA directly, or by interacting with other proteins that themselves control which genes are switched on.
For further information: http://www.arthritisresearchuk.org/about_us/arthritis_news/press_releases/2010/scientists_find_master_switch.aspx