Adding another incentive to exercise, scientists at Duke University Medical Center have found that physical activity improves arthritis symptoms - even among obese mice that continue to eat a high-fat diet. The insight suggests that excess weight alone isn't what causes the aches and pains of osteoarthritis, despite the long-held notion that carrying extra pounds strains the joints and leads to the inflammatory condition
Adding another incentive to exercise, scientists at Duke University Medical Center have found that physical activity improves arthritis symptoms - even among obese mice that continue to eat a high-fat diet. The insight suggests that excess weight alone isn't what causes the aches and pains of osteoarthritis, despite the long-held notion that carrying extra pounds strains the joints and leads to the inflammatory condition.
!ADVERTISEMENT!
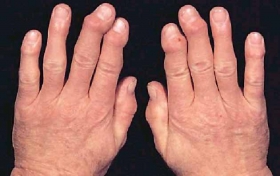
Arthritis is a form of joint disorder that involves inflammation of one or more joints.
There are over 100 different forms of arthritis. The most common form, osteoarthritis is a result of trauma to the joint, infection of the joint, or age. Other arthritis forms are rheumatoid arthritis, psoriatic arthritis, and related autoimmune diseases. Septic arthritis is caused by joint infection.
Regular, moderate exercise offers a whole host of potential benefits to people with arthritis. Mainly, exercise reduces joint pain and stiffness, builds strong muscle around the joints, and increases flexibility and endurance. It reduces inflammation from arthritis and related conditions and reduces the risk of other chronic conditions.
Published September 27 online in the journal Arthritis & Rheumatism, the new findings are now being tested in people.
"What's surprising is that exercise, without substantial weight loss, can be beneficial to the joints," said Farshid Guilak, PhD, professor of orthopaedic surgery at Duke and senior author of the study.
Even modest improvements could have a major impact if the findings are borne out in people. The Arthritis Foundation reports that one in five adults in the United States have been diagnosed with arthritis, and the annual cost of treating it and other rheumatic conditions has been tabbed at $128 billion.
Many cases of arthritis are associated with obesity and inactivity, so the Duke researchers set out to determine whether a high-fat diet induces knee osteoarthritis, and then whether exercise provides a protective effect.
Using two sets of male mice -- half fed a high-fat diet and the other fed regular food - the researchers noted significant differences between the two groups. The mice on the high-fat food gained weight rapidly, processed glucose poorly, and had much higher blood levels of molecules that trigger the chronic inflammation associated with osteoarthritis.
But when these animals got regular running wheel workouts, many of the harmful effects diminished - even though the mice ate the same high-fat food and shed no weight. Glucose tolerance improved, while the inflammatory response was disrupted among key signaling molecules called cytokines, easing the development of arthritis.
If the extra weight on the joints had been the cause of the arthritis, the researchers noted, exercise would have exacerbated the problem. Instead, it helped.
The findings add to a growing body of research exploring fitness vs. fatness. Ongoing studies at Duke and elsewhere are examining the role of diet, exercise, and inflammatory diseases.
For further information: http://www.dukehealth.org/health_library/news/exercise-eases-arthritis-in-obese-mice-even-without-weight-loss
Photo: http://westorlandonews.com/wp-content/uploads/2010/10/arthritis.jpg